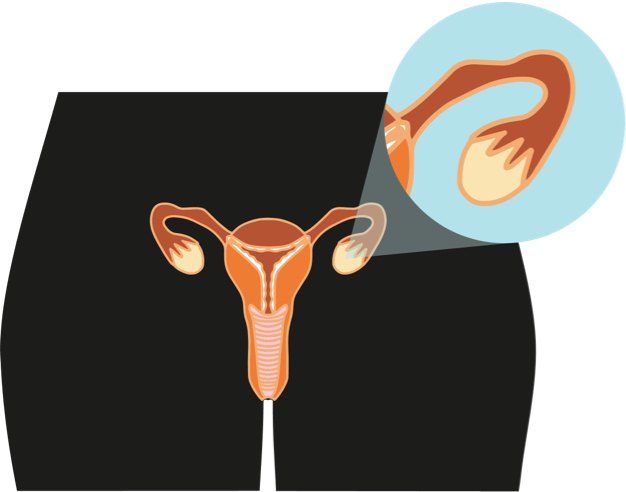
The symptoms of ovarian cancer can be vague and seem a bit like some other conditions. There are a number of symptoms to look out for, including:
- bloating in the belly or increased size around your belly
- feeling full quickly or not feeling like eating
- pain in the belly or in the pelvis
- change in toilet habits, such as constipation or feeling like you need to wee more frequently
- feeling very tired
- putting on or losing weight for no reason.
If you have any of these problems, especially if they are unusual for you or persistent, yarn with your doctor, nurse or Aboriginal and/or Torres Strait Islander health worker.
There is no screening test for ovarian cancer.