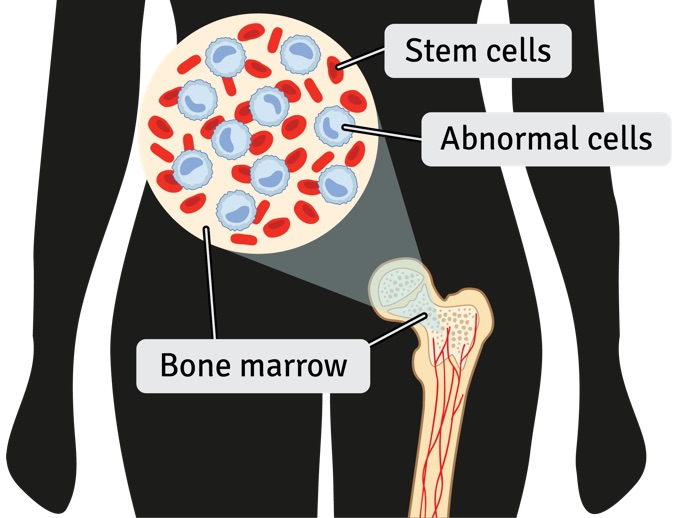
Sometimes people have found out that they had leukaemia without ever knowing there was a problem, until they saw their doctor for something else.
However, there are a number of symptoms you should look out for, including:
- feeling really tired or short of breath
- low levels of iron in the blood (anaemia)
- sepsis, also known as blood infection
- infection or high temperature that doesn’t get better
- abnormal bleeding/bruising that is unusual for you
- sore or bleeding gums that don’t get better
- bone pain that you can’t explain
- losing weight without meaning to
- swollen belly
- lumps or swollen lymph nodes
- night sweats.
Having these symptoms may not mean you have cancer, but it is important to check.
If you have any of these problems, or are worried about something else, yarn with your doctor, nurse or Aboriginal and/or Torres Strait Islander health worker.